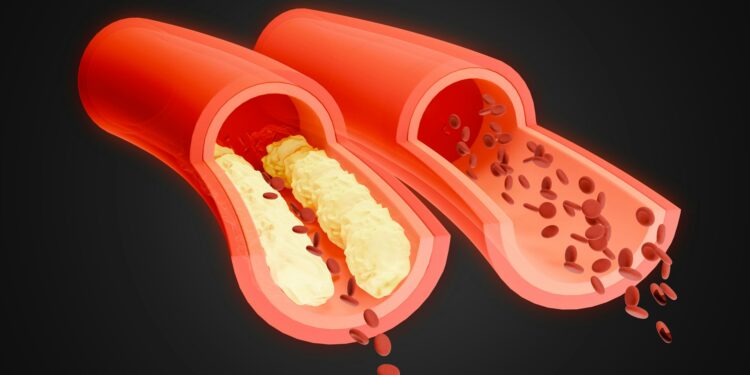
Throughout his career Charles V. Pollack, MD has been very active in the area of cardiovascular emergencies, especially in study of remedies for diseases of the blood and blood-clotting disorders. Blood clotting, or coagulation, is the process where proteins and platelets come together to stop too much bleeding and to help heal a cut, wound or damage. Usually, after the injuries heal, the body will gradually and effortlessly eliminate clots. However, certain circumstances and issues might cause a clot to not dissolve or form needlessly which can cause numerous health conditions and life-threatening medical catastrophes. The Centers for Disease Control and Prevention (CDC) has identified many risk factors that may raise a person’s risk for major blood clots such as deep vein thrombosis (DVT) and pulmonary embolism (PE).
Sometimes, once a person has an injury to a vein, a blood clot might form. Several types of injuries can damage veins, including fractures and severe muscle injuries. Other times, veins might sustain damage during major surgical procedures, especially those involving the legs, pelvis, hips, or abdomen.
Additionally, a condition or medical event that results in slowing the flow of blood raise a person’s risk for clots. This often occurs in situations that limit a person’s movement or confine them to a bed, meaning virtually any health issue that leads to long-term hospitalization or requires prolonged bedrest can increase the risk of a clot. Paralysis and casts that restrict limb movement can also heighten the risk. If a person must spend extensive time on bedrest or requires a treatment that limits mobility, they can discuss strategies for preventing blood clots with a medical professional.
Moreover, certain behaviors and non-medical circumstances can also slow down blood flow, such as sitting for long periods or leading an overly sedentary lifestyle. Movement in the legs causes calf muscles to contract, which promotes blood flow. The lack of contraction from sitting for hours without moving can slow blood flow, especially when sitting cross-legged. Beyond a sedentary lifestyle, inactivity that may elevate blood clot risk include lengthy travel by car or plane and jobs that require sitting for prolonged periods.
Certain chronic medical conditions place patients in a hypercoagulable state that makes blood clot more easily, leading to a higher risk of unnatural blood clots. A few of these include heart disease, lung disease, and inflammatory bowel disease. Tobacco use independently increases the risk of abnormal blood clotting. Some cancers and cancer treatments can increase risk, as well.
Finally, elevated levels of estrogen are correlated with a heightened risk of blood clots. A person may have high estrogen levels as a result of using contraceptives containing estrogen or receiving hormone replacement therapy, the latter of which some women undergo after menopause. Estrogen levels also increase during pregnancy and remain elevated for up to three months following delivery.
While these factors raise the chances of a blood clot, anyone can develop a DVT or PE. Additionally, having multiple factors at once elevates the risk even further. For example, while a long plane flight alone might not appreciably impact DVT risk, a long plane flight for a cigarette smoker who is also taking hormone replacement therapy with estrogen is more likely to precipitate a clotting problem. With this in mind, Charles V. Pollack, MD, and other experts recommend people listen to their bodies and discuss their potential DVT and PE risks and worrisome symptoms with a medical provider, as both conditions can rise in severity over time.